Answer: Death of dopamine cells in the substantia nigra leads to changes in the output of the striatum.
Credit: https://www.frontiersin.org/articles/10.3389/fnana.2015.00005/full
Parkinson’s disease is a movement disorder characterized by resting tremor, difficulty initiating movement, and a shuffling gait. It is generally diagnosed in old age, with an estimated prevalence of 1 in 100 over the age of 60. A small fraction of cases are early onset, and these cases are closely tied in with a genetic component.
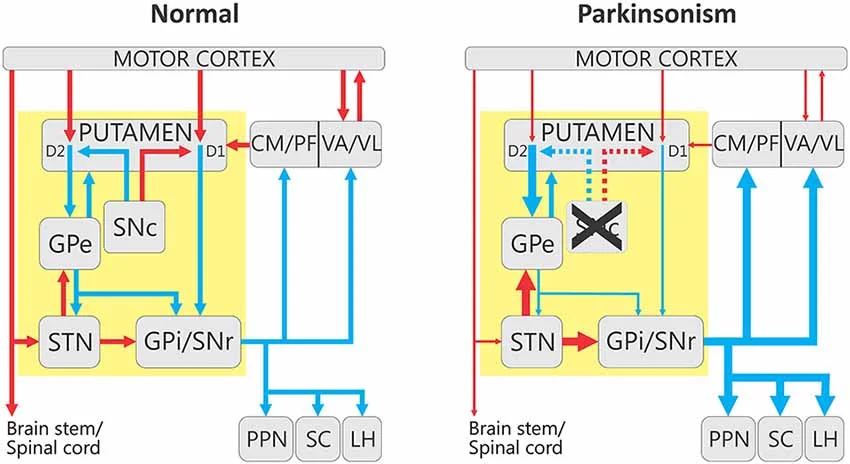
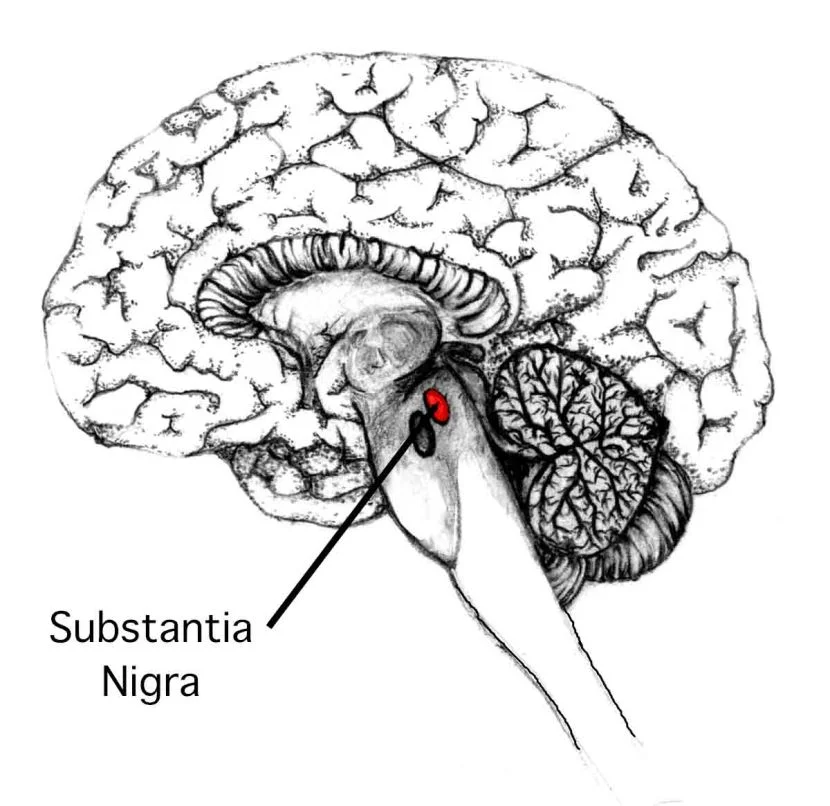
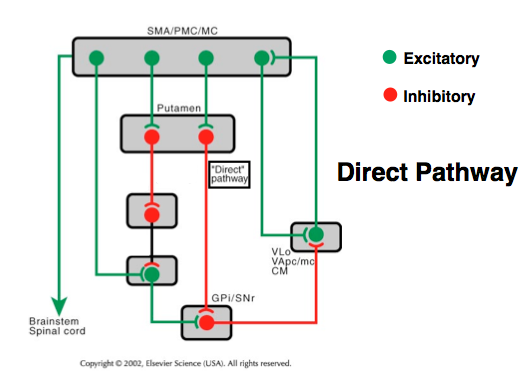
The substantia nigra is a brain region that sends dopamine projection neurons into the striatum. Within the striatum, there are two populations of cells that send their axons outside of the striatum: the direct pathway medium spiny neurons and indirect pathway medium spiny neurons.
Activation of the direct pathway neurons promotes motor activity, while activation of the indirect pathway neurons inhibits motor activity. In the non-Parkinsonian state, dopamine excites the direct pathway neurons and inhibits the indirect pathway neurons. When the dopamine cells die in Parkinson’s disease, this circuit is disrupted. Patients with Parkinson’s exhibit their symptoms because of the decreased excitation of the direct pathway neurons, and disinhibition of the indirect pathway neurons.
Dopamine acts on the direct pathway neurons by activating dopamine D1 receptors. These receptors are linked to Gs proteins, which stimulate cell activity through activation of adenylyl cyclase. On the other hand, dopamine acts on indirect pathway neurons by activating dopamine D2 receptors. These receptors are coupled to Gi proteins, which inhibit cell activity by decreasing adenylyl cyclase activity. The D1 and D2 receptors are expressed on two separate populations, which means that a change in dopaminergic tone alters the output of the striatum.
The symptoms of Parkinson’s disease are treated with L-DOPA.