Answer: Acetylcholinesterase is an enzyme that breaks down the neurotransmitter acetylcholine.
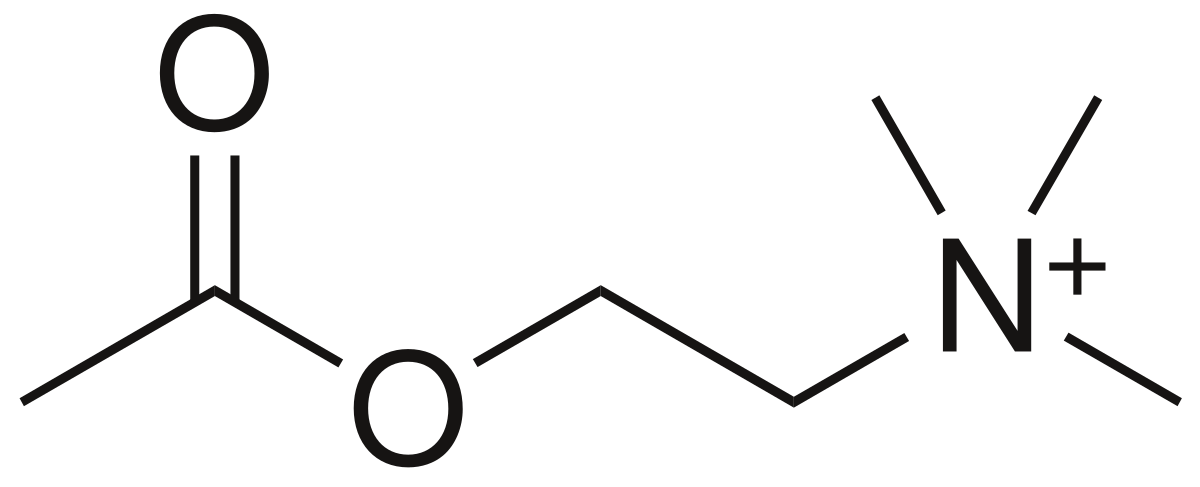
Acetylcholine, the substrate of acetylcholinesterase.
Acetylcholine is a neurotransmitter and neuromodulator that is released at synapses in the brain and neuromuscular junction in the periphery. Substances that are released into the synapse activate postsynaptic receptors, and will continue to do so with stochastic probability. In some cases, this signal ends when the neurotransmitter is transported into the presynaptic membrane by a process called reuptake. In the case of acetylcholine, the signal ends when the enzyme acetylcholinesterase degrades the neurotransmitter remaining in the synapse.
Acetylcholinesterase is an extremely rapidly acting enzyme. It is estimated that a single molecule of AChE can break down 25,000 molecules of acetylcholine per second, making it among the fastest acting enzymes in the body. Because of how quickly the enzyme works, a signal at a brain synapse or neuromuscular junction can be terminated very rapidly.
Acetylcholinesterase degrades ACh by hydrolysis, the biochemical process in which a water molecule is added to the substrate. The final products of acetylcholine hydrolysis are choline and acetate. From here, the choline molecules undergo reuptake into the presynaptic terminal. They combine with Acetyl-CoA due to the action of choline acetyltransferase to form acetylcholine, which is then repackaged into vesicles.
Acetylcholinesterase inhibitors
Acetylcholinesterase is inhibited by the action of organophosphate toxins and nerve agents, such as tabun, sarin, and VX. With nerve gases, the most common cause of death is asphyxiation. The involuntary muscles that control movement of the diaphragm is what allows for a person to inhale and exhale, getting the oxygen into their bodies. However, in the presence of the acetylcholinesterase inhibitor sarin, the acetylcholine is not broken down and the muscles continue to contract without allowing relaxation of the diaphragm.
Acetylcholinesterase inhibitors can also be used therapeutically in a few cases. For one, treatment of myasthenia gravis, a neurological disease that results from destruction of nicotinic acetylcholine receptors. Myasthenia gravis is an autoimmune disorder that results from some antibodies that specifically target and destroy the normal complement of receptors that are expressed in the periphery at the neuromuscular junction. In a person with myasthenia gravis, they have profound muscle weakness, predominantly in the facial muscles. As a result, they may exhibit eyelid drooping and a difficulty with focusing. Because cholinergic signaling is lowered in these people, administering a cholinesterase inhibitor can increase the amount of acetylcholine that remains in the synapse, which can help reverse the muscle weakness the patients experience. Neostigmine is a common acetylcholinesterase inhibitor that is prescribed to these patients.
Acetylcholinesterase inhibitors are also used therapeutically to possibly alleviate some of the symptoms of Alzheimer's disease. One major theory that was put forward to explain the symptoms of Alzheimer’s disease was that there is a decrease in acetylcholine in the basal forebrain. According to this theory of Alzheimer’s disease, by giving doses of the acetylcholinesterase inhibitor rivastigmine, the brain will increase the level of cholinergic innervation that was lost in the disease.