Answer: Urbach-Wiethe disease is a rare genetic disease that can have neurological side effects such as specific destruction of temporal lobe structures.
Urbach-Wiethe disease was first characterized in 1929 by two Austrian physicians, Erich Urbach and Camillo Wiethe. It is an autosomal recessive disease that presents itself at early childhood. It is sometimes called lipoid proteinosis. The prominent dermatological symptoms include a hoarse voice, slow healing of injuries on the skin, hair loss, and often beading of papules around the eyes. The skin may be easily damaged, and the scarring that occurs may leave the skin with a waxy appearance. In early childhood, Urbach-Wiethe disease may lead to an enlargement of the tongue, increased thickness of the mucus membranes, and changes in the pharynx, possibly affecting respiration at early ages. But generally, Urbach-Wiethe disease does not cause any significant changes in lifespan. There is currently no known cure for the disease; the dermatological symptoms are manageable in early childhood.
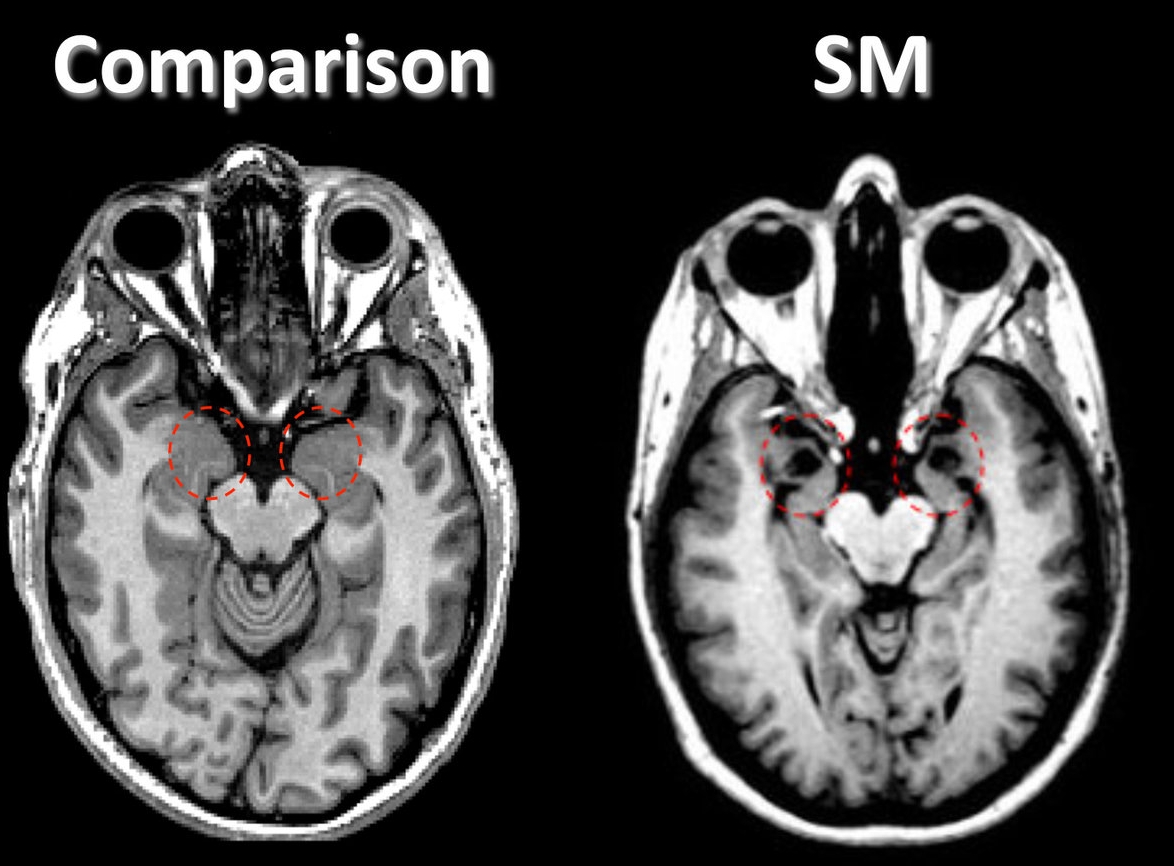
Urbach-Wiethe disease may also present itself neurologically. In particular, the medial temporal lobes are most heavily affected by the disease. Blood vessels that feed into these brain regions can develop calcifications, and these contribute to the formation of lesions as the blood vessels harden and die. In particular, the amygdala and periamygdalar gyri are sensitive to these lesions. The amygdala is known to play a role in processing and understanding emotionally related memories, as well as processing the understanding of fear.
One patient who was studied for her neuorological damage following Urbach-Weithe disease was Patient SM. She had significant damage to her amygdala as a result of the disease. She has been an important case study towards improving our understanding of amygdala function. In the laboratory setting or in real life, she displayed no signs of experiencing fear. For example, she was taken to a haunted house as part of an experiment, and did not react to any of the surprising fearful stimuli as expected. Instead, she wanted to talk to and touch the actors who were dressed as various monsters. Patient SM, under supervision of the laboratory that was running the behavioral tests on her, went to any pet store where she was asked to hold various animals that might trigger anxiety or fear in other subjects, such as a snake and a spider. She described the experience as mostly driven by curiosity. In real life, she recalled an incident where she was held up by a man with a knife. She displayed no fear during the incident, and even returned to the same location the next day.
Urbach-Wiethe disease can also present other neurologically relevant symptoms. One other symptom that may appear in the disease is epilepsy. The temporal lobes are often where the focus of epileptic activity is located. Aside from the epilepsy, patients may experience schizophrenia or anxiety like symptoms.
It is estimated that only 400 cases of Urbach-Wiethe disease has been reported. Interestingly, about one-fourth of all cases have been reported in South Africa. Being an autosomal disease, it is generally seen in families. Lipoid proteinosis: case report and review of the literature.
Mechanism of Urbach-Wiethe disease
The biological genetic changes observed in Urbach-Wiethe disorder have been traced to a glycoprotein called the extracellular matrix protein 1 (ECM1). The gene that codes for this protein is located on chromosome 1.
It is still unclear what the function of ECM1 is in the normal human. In loss-of-function experiments where protein levels are decreased, it was observed that there were deficits in wound healing.
Many of the dermatological symptoms may be a result of the infiltration of a glassy, proteinaceous substance called hyaline. The hyaline material can aggregate around the blood vessels and in some internal organs. Sometimes, the hyaline can affect the eyelashes, causing a prevention of hair growth (alopecia) or a corneal abrasions. (Urbach–Wiethe disease)